He can help you manage pain
August 2, 2019
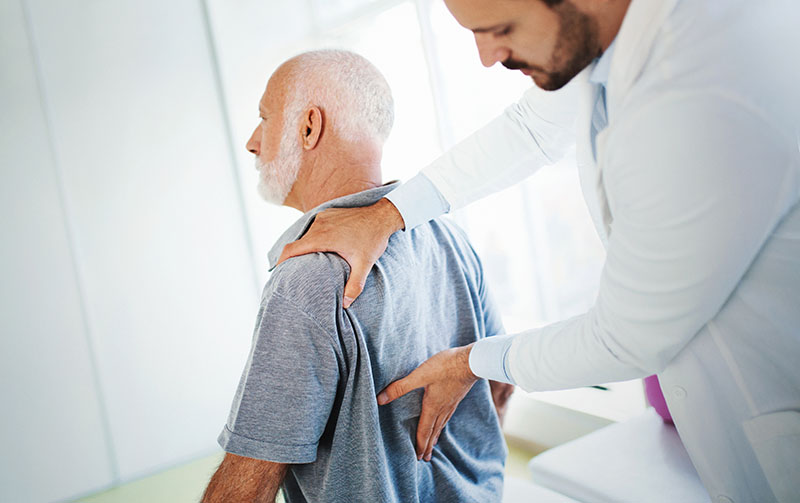
Nationally recognized Pain Management Specialist George Macrinici, M.D. answers questions about his role at NCH to help patients improve function and quality of life.
What types of conditions do you treat?
I treat all pain conditions including lower back, pelvic, post-surgical, neck, traumatic injury, hip, knee and shoulder pain, diabetic nerve pain, degenerative discs, shingles, sciatica, spasticity and neuropathic pain, and headache.

What kind of training/expertise do you have?
I’m a nationally recognized pain physician who has won multiple professional awards including “Best of Meeting Award” from the American Society of Regional Anesthesia and Pain Medicine (ASRA) in 2016 and the North American Neuromodulation Society (NANS) Fellow title in January 2018. I’m triple board-certified in Pain Medicine, Anesthesiology and Spinal Cord Injury Medicine. I have extensive experience as an anesthesiologist, in interventional surgery, cancer pain management and private practice. I’m a member of ASRA, NANS, the American Society of Anesthesiology and the American Spine Injury Association.
What should patients know about pain management?
1) Patients with pain do not need to suffer.
2) There are many options for managing pain.
3) They do not need to go to the city for pain management. We provide the same level of expertise at NCH.
What are the latest procedures in pain management?
There are neuromodulation therapies that are very effective at managing pain. The newer spinal cord stimulators (SCS) are used to mimic the actual nerve conduction in the spine and can greatly minimize pain. Initially, we conduct a trial by inserting some tiny wires into the epidural space and connecting them to an external battery. The patient goes home for seven days and then returns to the office to report on whether or not it’s working for them. If the patient decides they would like to move to the second stage, I take them to the operating room to implant wires connected to a battery under the skin and subcutaneous fat. The batteries we have today last for five to seven years, and exchanging the battery involves minimal discomfort. The patient goes home with markedly reduced pain and can live their life without suffering.
What type of patient does SCS help?
Patients who have had chronic neuropathic pain for years. I have had patients who’ve tried everything and gone through a lot of pain doctors for many years until they got this form of neuromodulation therapy. Many patients can finally sleep without waking up during the night due to an implanted spinal cord stimulator.
Are there other neuromodulation therapies?
We offer a dorsal root ganglion stimulator or DRG. It’s an FDA-approved device that offers superior pain relief for localized pain. For example, sometimes a patient who has had a knee replacement might end up with disabling, localized pain. A DRG implant helps. One of my patients who had it done recently is finally returning to work for the first time after several years of suffering debilitating pain.
There’s also a pain pump that often can help reduce a patient’s severe pain level down to a minimal pain level. That’s a good, stable result and it’s amazing.
How does a pain pump work?
We implant it under the skin, connect it to the spine with tubing, and it delivers pain medication directly to the spine where pain fibers converge. In patients who are afraid of addiction caused by high-dose narcotics, this is a good choice. The pain pump gives the equivalent of 300 mg of oral morphine, but it’s actually only 1 mg given into the spine. Patients don’t suffer the terrible side effects, they can drive while getting the medication and they can live their lives. Moreover, the patient can dose themselves every two hours, which is safer than taking oral medications. I would strongly recommend this option for patients who have spasticity (stiffness/spasms that won’t go away).
What can a patient expect at a first visit?
The patient is registered, we gather all their medical information, we listen to them and I examine them. I always ask the patient what they are looking for and find out what their expectations are. I lay out all the options and send them home with medical information to read so that they can make an informed decision.
How do you feel about prescribing pain medication such as opioids?
Giving out high-dose narcotics is not the answer to chronic pain. I’ve never seen a patient have a good result from taking just opioid medications. A good portion of opioid-addicted patients started their suffering after being prescribed narcotics for acute postoperative pain. It’s important to have a pain management doctor as part of the multidisciplinary team to treat these patients, starting prior to surgery since there’s a direct correlation between pain before – and after – surgery. We must correctly assess these patients and have a plan in place for after surgery to safely wean them off medications.
Dr. Macrinici practices at 1100 West Central Road, Suite 305 in Arlington Heights. To schedule an appointment, call 847-797-4888.
Most insurance, including Medicare, is accepted. A referral from your primary care provider might be needed.