Jose’s journey
July 23, 2020
Most people associate strokes with senior citizens, but sadly they can happen to anyone of any age at any time. Fortunately, we have the tools to help patients live their lives to the fullest after a stroke.
Early in March Jose was diagnosed with acute hypertension and diabetes. The 33-year-old Mount Prospect resident works full-time in a bakery and enjoys exercising and competitive wrestling. He lives with his wife and four children, ages 4 to 10. On March 5, Jose developed significant left-sided weakness and was unable to stand or walk. He was taken by ambulance to Northwest Community Hospital (NCH) where his symptoms had progressed to the point that he was unable to talk, eat or drink and he had lost all active movement on the left side of his body. He was diagnosed with an acute stroke that was most likely caused by uncontrolled hypertension.
After a week in the hospital, Jose was medically stable and was transferred to NCH’s John M. Boler Center for Rehabilitation, ready to begin his road back to independence. The impairments from the stroke had significantly impacted Jose’s ability to function. He was unable to eat a regular diet or communicate with ease. Jose could not sit unsupported, get out of bed, walk and perform self-care activities without the assistance of at least one other person.
Jose received occupational therapy, physical therapy and speech therapy for six days a week for nearly five weeks. The program was designed to meet Jose at his current functional level and challenge him just a little more each day. Jose benefited from the newest technologies with robotic and virtual reality treatment intervention. His nurses, specially trained in rehabilitation, helped him carry out what he learned during therapy the other 21 hours of the day, by encouraging him to use his stroke-impaired arm and leg while completing everyday tasks such as brushing his teeth, eating, dressing and walking.
Once a week the entire rehab team – doctor, nurse, therapists and social worker – met to discuss Jose’s challenges, offering ideas to help him progress, goals to be met for the week and plans for a safe discharge home.
The occupational therapist fabricated a custom left-hand resting splint to provide protection and ensure proper hand positioning when Jose slept. He was also given a shoulder sling to use when he walked to keep his left shoulder properly aligned. Jose was taught how to wear and remove the orthotics, when to wear them and how to care for them.
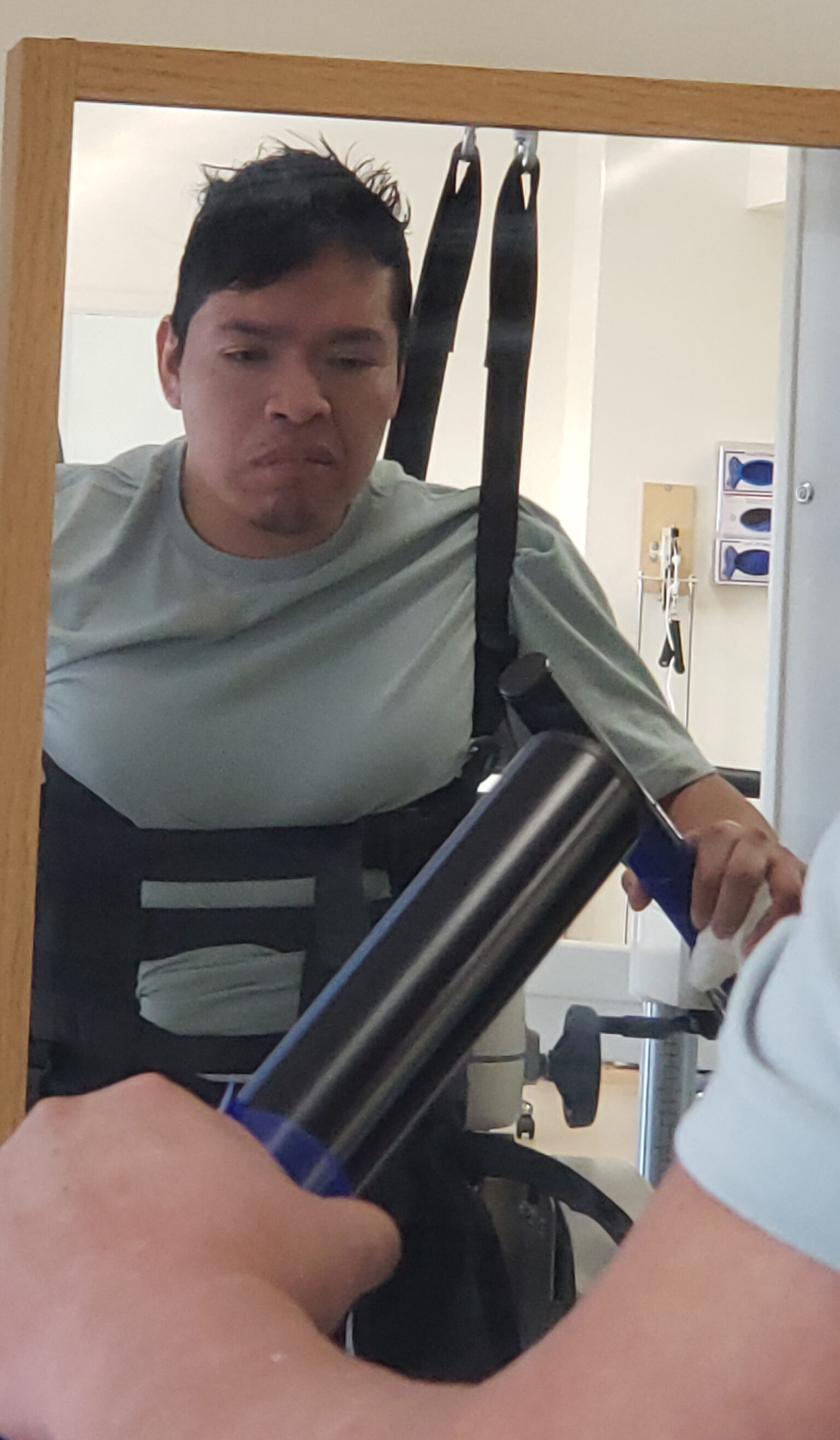
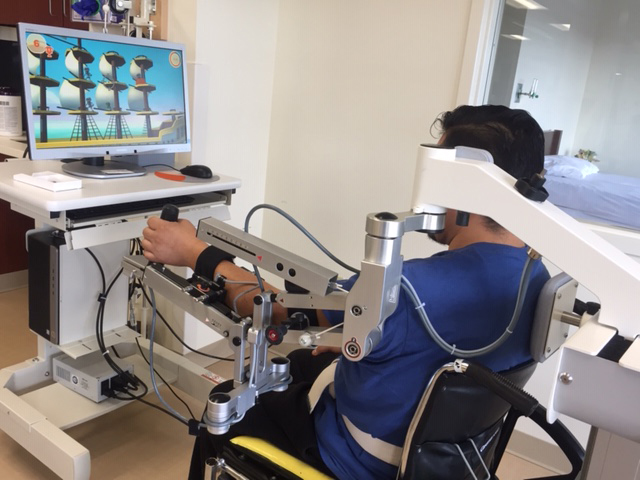
The occupational therapist used a variety of strategies and state-of-the-art technologies to help Jose regain the ability to complete activities of daily living (dressing, bathing and personal hygiene). Jose benefited from repeated use of the Robotic Armeo® Senso, equipment designed to enhance a patient’s arm movement and hand/eye coordination. It enables patients to participate in exercises that are self-initiated, self-directed, functional and fun.
The first week in physical therapy started slow and difficult as Jose needed the help of two people to start standing trials using the parallel bars. Early treatment focused on initiating leg strengthening and sitting balance to progress his mobility.
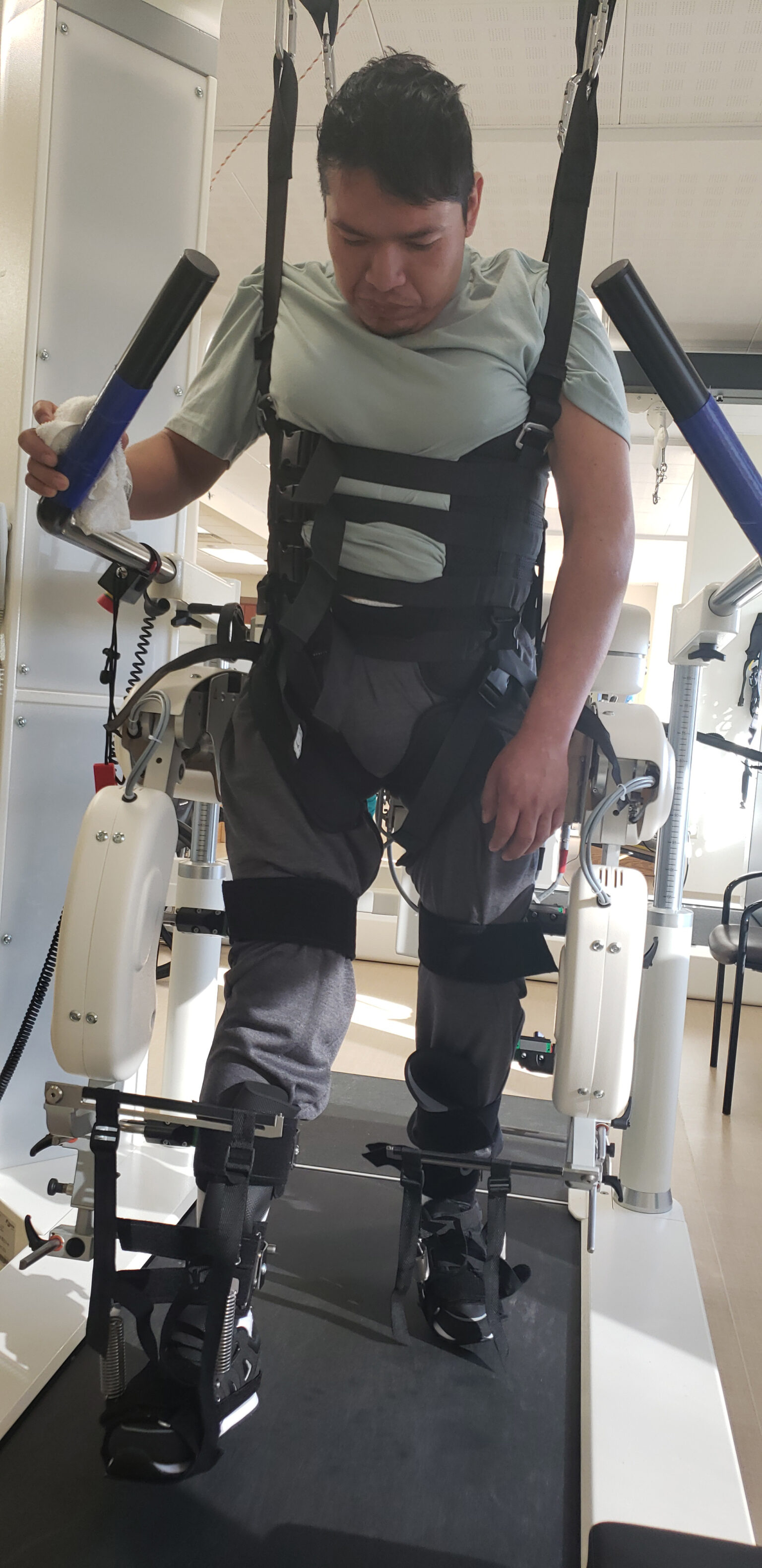
Jose was then introduced to the Lokomat®Pro, a state-of-the-art robotic treadmill training system. It uses a body weight support system to suspend individuals in robotic legs that assist with basic walking functions. After two sessions on the Lokomat, Jose began to have some active movement in his left hip and knee. He was ready to be trained to walk over ground using the Maxi Sky® harness with two people assisting him to advance his left leg with each step.
Just two weeks later, Jose began to have active movement in his left ankle and was able to stand, transfer and walk using a hemi-walker with minimal assist from his physical therapist.
Initially, Jose was on a modified diet of soft foods and nectar thick liquids. Jose’s speech was difficult to understand, and he had difficulties with some thinking skills. He worked with a speech language therapist and learned swallowing and facial strengthening exercises. Additionally, he worked to improve his memory and apply complex problem-solving skills to prepare for eventual return to work.
Jose attended the weekly “stroke education group” with other stroke patients to learn about the causes of a stroke, ways to prevent them and support groups available in the community. Jose and his wife participated in caregiver training provided by the nursing staff and therapists to prepare them both for a safe transition back home.
With the help of repetition, participating in progressively more complex demanding tasks and by learning new techniques, Jose was able to bathe, dress, eat and use the toilet independently by the time he was able to go home.
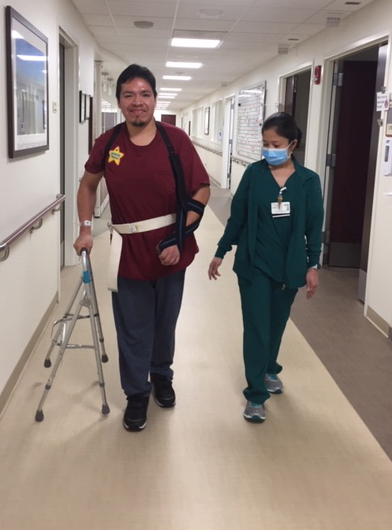
Jose completed his 34-day stay in rehab and was excited to return home to his wife and children. He was able to sit and stand without any help and walk approximately the length of a football field (347 feet) using a hemi-walker. He was able to transfer in and out of a bed and a car, go up and down 12 steps, manage a curb step and walk on uneven surfaces.
Although Jose’s journey to recovery continues at home, he made great strides at the Boler Center for Rehabilitation, regaining many lost skills and learning how move forward with his best possible quality of life.
The John M. Boler Center for Rehabilitation is located in Northwest Community Hospital at 800 W. Central Road, Arlington Heights, and is now accepting new patients. For more information about rehab services or to schedule an appointment, call 847-618-6716.
No case is the same, results may vary.